Four Stages of COPD
- Direct O2

- Apr 22, 2020
- 4 min read
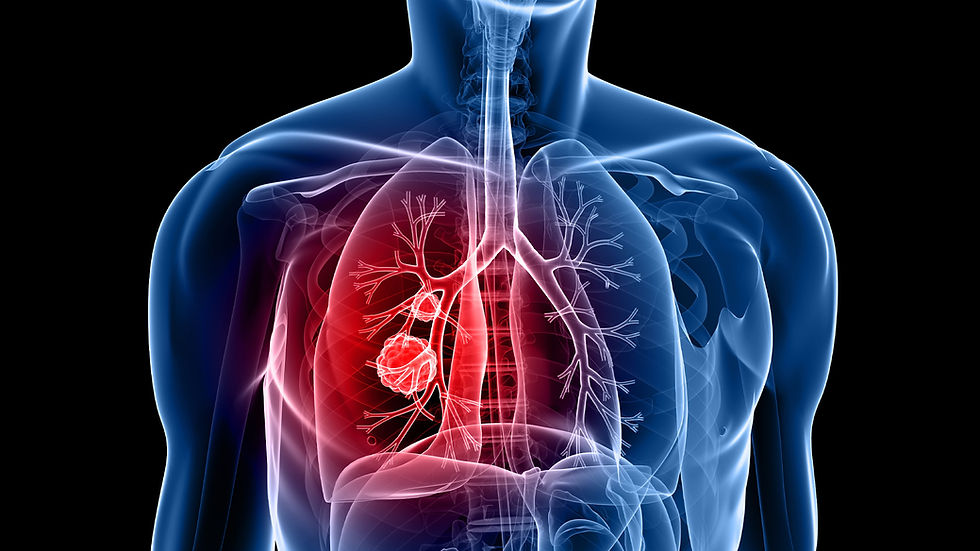
Chronic obstructive pulmonary disease (COPD) is a chronic lung disease that progressively restricts airflow in and out of the lungs. COPD makes it more and more difficult to breathe. A majority of COPD cases are caused by smoking tobacco, but some other causes can be

long-term exposure to air pollution or genetic disorders involving a protein deficiency. Constant coughing, wheezing, and shortness of breath are symptoms that can sometimes go unnoticed until the later stages of COPD. Early detection is vital in slowing its progression and managing the symptoms.
Doctors use four stages to describe the severity of COPD, allowing them to provide the most appropriate treatments for each stage.
So what are the stages of COPD?
Stage I: Early
When COPD first appears, it is very gradual and often takes years to progress, but by the time a patient has symptoms, they typically have already experienced lung damage. That’s why it’s so important to keep an eye out for early signs if you’re at risk for COPD!
Typically, COPD starts with a nagging cough that can be dry or contain mucus. You may also notice shortness of breath when you exert yourself.
What will the doctor do to test me for COPD? It can be easy to ignore the early symptoms of COPD or simply assume they are just part of getting older. The best thing to do is tell your doctor if you have breathing symptoms, especially if you have been a smoker at any time in your life or worked in an environment with bad air quality. The best treatment for COPD is to catch it early! Slowing the progression of the disease will allow you to enjoy the fullest health possible. Your doctor may perform tests to confirm the presence of COPD:
1. A simple physical exam

2. Spirometry: Your doctor will ask you to take a deep breath in and blow hard into a tube connected to a spirometer machine. This will measure how well your lungs are working.
3. Your doctor may also perform an alpha-1-antitrypsin (AAt) deficiency test.
4. Chest X-ray or CT scan, other lung tests
5. A 6-minute walk test
6. or blood tests.
Stage II: Moderate
As COPD progresses, it will start to affect your day-to-day life. Because of this, it’s the most common phase when people go to the doctor.
What Are the Symptoms of Stage II COPD? Stage II is the natural progression of stage I symptoms, including:
Frequent or constant coughing that contains mucus (usually worse in the morning)
Feeling tired
Shortness of breath that makes common activities a challenge
Trouble sleeping
Wheezing
You may also feel forgetful, confused, or have slurred speech.
You have stage II if your FEV1 (forced expiratory volume in 1 second, measured during a spirometry test) is between 50% to 80% of the normal value for someone of your age, sex, height and race.
During stage II, you may also start to have flare-ups, called exacerbation's, when your symptoms intensify for a few days. At this point, your doctor may prescribe bronchodilators, which help make breathing easier. They may also refer you to pulmonary rehabilitation.
Stage III: Severe
During stage III of COPD, patients experience intensified symptoms, such as intensified shortness of breath, coughing and tiredness as well as more frequent flare-ups.

Typically, you will also experience new signs of COPD progression, including getting colds more often, feeling tightness in your chest, swelling in your ankles and feet, having trouble catching your breath, and breathing issues when you exert yourself. Although your symptoms may have gotten worse, it’s important to stay active and pursue a healthy lifestyle to minimize COPD’s progression.
If you have not already completed a pulmonary rehabilitation program, ask your doctor for a referral. Pulmonary rehabilitation includes exercise training classes, with expert therapists, and is one of the most effective treatments available for alleviating your symptoms.
Stage IV: Very Severe
During stage IV of COPD, your quality of life will be lower, as your COPD begins to more greatly affect every activity. It will be difficult to breathe even without exertion.
Chronic respiratory failure can also occur, in which not enough oxygen moves from your lungs into your blood or when your lungs don’t take enough carbon dioxide out of your blood.
You doctor may prescribe supplemental oxygen to help with your breathing. At this point, other treatment options include surgery, having special valves implanted into your lungs, or lung transplantation.
What can I do today to limit the progression of COPD?
If you are able to catch COPD early, your doctor might prescribe a short-acting bronchodilator (inhaler) to use as needed that lessens the symptoms you are feeling.

To add to this treatment, there are some other preventative steps you can take toward living a healthier, better lifestyle:
Get your yearly flu and pneumonia shots. These vaccines will boost your immune system and protect your body against additional diseases and conditions.
Consider your environment. If you work somewhere with high amounts of pollution, it might be best to take a step back and reevaluate the risks. Avoiding triggers like dust, pollen, pollution, smoke, perfumes, and working or cleaning with strong chemicals will actively lessen the symptoms of early-stage COPD.
Make the switch to a healthier diet. Consuming mainly healthy foods and getting enough vitamins will keep your body feeling strong and resilient.
Increase your exercise routine. Leading an active lifestyle gives your immune system that necessary support it needs to fight off COPD symptoms. It strengthens the muscles around your lungs for better breathing and improves how your body uses oxygen.
This BLOG was in part published by www.perf2ndwind.org




My Myasthenia Gravis (MG) symptoms started at the age of 51, I have had countless plasma exchanges as my veins are bad. I also needed Hickman lines inserted. I have been on azathioprine, mycophenolate (CellCept), methotrexate and none have worked. I'm currently done with my herbal remedy I purchased from multivitamin cure which has totally cured my condition with a surprise after almost four months of their usage, I was discouraged and never thought I would be myasthenia gravis (MG) free today,to me the best way to get rid of this condition is multivitamin cure herbal recommendation because all medications I used never worked include mycophenolate (CellCept),contact the multivitamincare .org today Call Us (or SMS): +1 (956) 758-7882 to lear…